What is Hyperthyroidism?
Commonly referred to as an overactive thyroid, hyperthyroidism is a condition where the thyroid gland produces excess thyroid hormones (T4 and T3), accelerating metabolism and overstimulating many body systems. It is a disorder of the endocrine system, which releases hormones directly into the bloodstream.
Understanding Hyperthyroidism
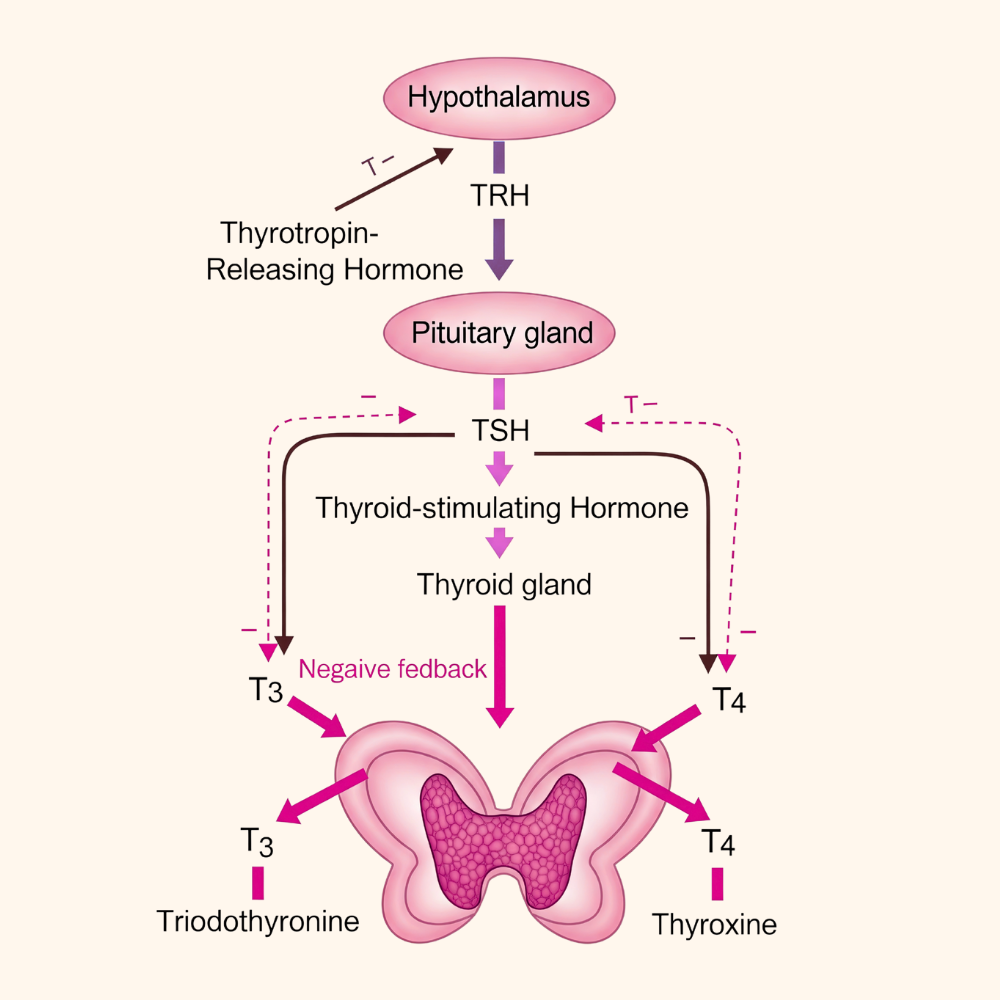
The thyroid gland, situated at the front of the neck, produces the thyroid hormones triiodothyronine (T3) and thyroxine (T4). Normally, the pituitary gland secretes TSH, which signals the thyroid to produce T3 and T4. Iodine is a key mineral used by the thyroid to synthesise thyroid hormones. Iodine is absorbed from food (like seafood, dairy, iodised salt). It travels through the bloodstream to the thyroid gland, where it is concentrated and combined with the protein thyroglobulin. Enzymes release T3 and T4 into circulation, and elevated levels increase the body's basal metabolic rate, raising heart rate, body temperature, and energy use. The pituitary gland responds to circulating hormone levels by reducing thyroid‑stimulating hormone (TSH).
However, in hyperthyroidism, the thyroid makes too much T3 and T4 (often due to Graves' disease antibodies or nodules), which strongly inhibits the pituitary gland, causing TSH levels to drop very low (suppressed). Despite low TSH, the thyroid continues to release excessive hormones, continuing the cycle of low TSH and high T3 and T4.
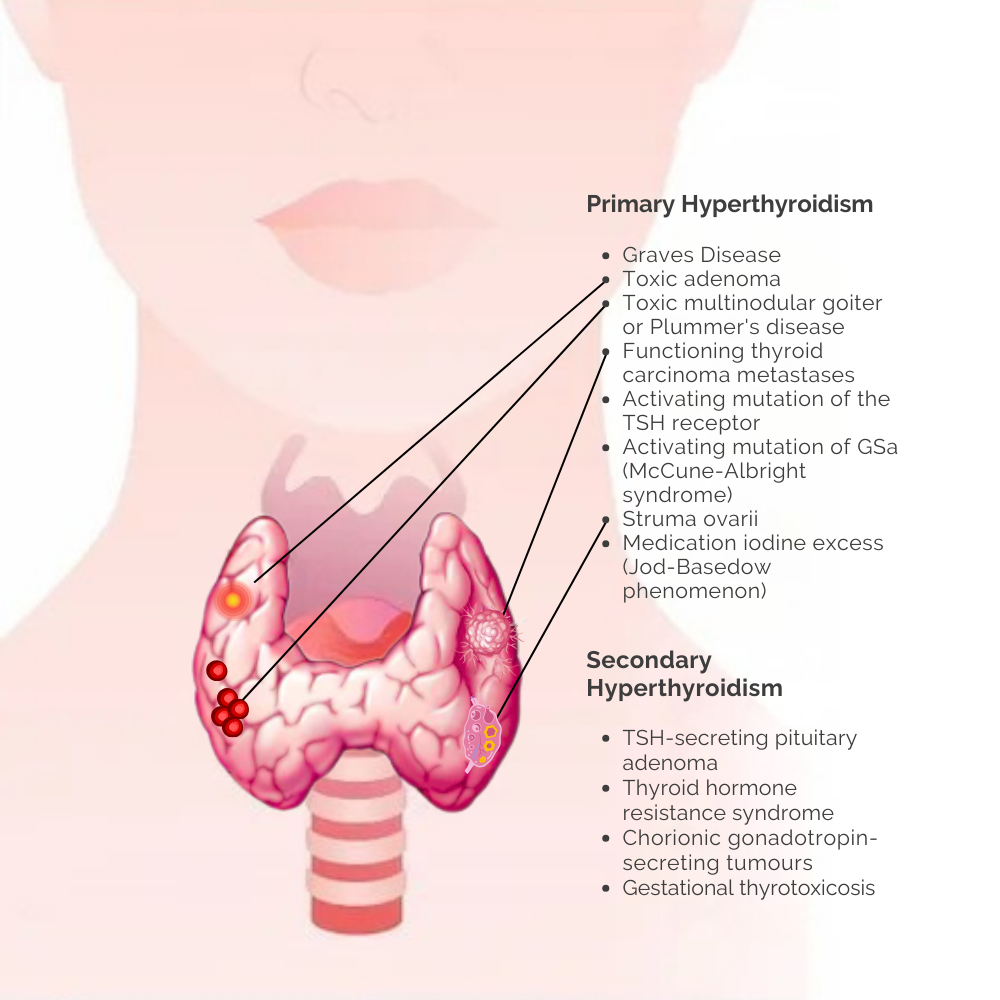
Causes of Hyperthyroidism
Several factors may trigger an overactive thyroid, including:
- Graves’ disease:
- An autoimmune condition where thyroid‑stimulating immunoglobulins activate the TSH receptor (~70–80 % of cases).
- Toxic multinodular goitre (Plummer’s disease):
- Autonomous hormone‑secreting nodules within an enlarged thyroid.
- Toxic adenoma:
- A single “hot” nodule producing hormones independently.
- Thyroiditis:
- Transient inflammation (sub‑acute, silent/post‑partum) causing hormone leakage.
- Excess iodine exposure:
- Contrast dyes, amiodarone, or high‑dose kelp supplements.
- Medication‑induced:
- Amiodarone, lithium withdrawal, interferon‑α.
- Pituitary adenoma or hCG‑mediated stimulation:
- Rare.
Signs and Symptoms of Hyperthyroidism
Symptoms vary with age, severity and duration, yet commonly include:
- General Changes
-
- Unintentional weight loss despite increased appetite
- Heat intolerance and excessive sweating
- Fatigue yet difficulty sleeping
- Cardiovascular Symptoms
- Resting tachycardia (> 100 bpm) or palpitations
- Atrial fibrillation, high pulse pressure, breathlessness
- Ocular (Graves’ ophthalmopathy)
- Gritty, dry eyes; photophobia
- Periorbital swelling; exophthalmos (bulging eyes)
- Reproductive & Hormonal
- Irregular or light menstrual cycles
- Reduced fertility or libido
- Neurological and Physiological
- Anxiety, irritability, mood swings
- Fine hand tremor, hyperreflexia
- Difficulty concentrating (“brain fog”)
- Dermatological
- Warm, moist skin; thinning hair; brittle nails
- Graves’ dermopathy (pretibial myxoedema)
- Gastrointestinal and Metabolic
- Increased bowel motions or diarrhoea
- Frequent thirst and urination
- Muscle weakness, especially proximal muscles
If left untreated, severe thyrotoxicosis can progress to a thyroid storm - a life‑threatening emergency featuring fever, delirium and cardiac failure.
Diagnostic Testing
To diagnose hyperthyroidism, doctors and naturopaths rely on a combination of blood tests and imaging studies to assess thyroid function and identify underlying causes. Key diagnostic methods include:
A comprehensive thyroid panel and targeted imaging help determine cause and severity:
- Blood Tests
- TSH – typically suppressed (< 0.01 mIU/L)
- Free T4 and Free T3 – elevated; T3‑to‑T4 ratio may point to Graves’ disease
- Thyroid‑stimulating immunoglobulin (TSI / TRAb) – positive in Graves’ disease
- Thyroid peroxidase (TPO) & thyroglobulin antibodies – assess autoimmune activity
- Complete blood count, liver function, ferritin – monitor systemic effects and treatment safety
- Imaging
- Thyroid ultrasound – assesses gland size, nodularity and blood flow
- Radioactive iodine uptake (RAIU) or technetium scan – differentiates diffuse uptake (Graves’) from focal (“hot”) nodules or thyroiditis
- Additional Investigations
- ECG for arrhythmias
- Bone mineral density in prolonged hyperthyroidism due to osteopenia risk
Interpreting the Results
Consulting a healthcare professional is essential for interpreting your results. Results such as in this example may guide ongoing management:
- Low TSH + Normal Free T3 + Normal Free T4 = Mild Hyperthyroidism
- Low TSH + High or Normal Free T3 + High or Normal Free T4 = Hyperthyroidism
- Positive Thyroid-Stimulating Hormone Receptor Antibodies (TRAb) = Graves' Disease
- Positive Thyroid-Stimulating Immunoglobulins (TSI) = Graves' Disease
Naturopathic Approaches to Hyperthyroidism
At All Naturopath Surrey Hills, we emphasise individualised care, focusing on natural therapies and lifestyle modifications to restore thyroid function. Key strategies include:
- Nutritional Support: Following an anti-inflammatory, antioxidant diet with abundant colourful vegetables and berries, oily fish, olive oil, and green tea, with a moderate amount of iodine (unless otherwise directed), is supportive of hyperthyroidism.
- Herbal Medicine: Bugleweed (Lycopus europeus), Lemon balm (Melissa officinalis), and Motherwort (Leonurus cardiaca) have been traditionally used to support an overactive thyroid. These herbs may help reduce tachycardia and palpitations, soothe tremors and anxiety, but are best for the subclinical presentation of Graves. It's essential to consult with a qualified naturopath before starting any herbal regimen.
- Addressing Nutrient Deficiencies: Selenium, vitamin D, and ferritin deficiencies worsen hyperthyroid symptoms and autoimmune activity by driving oxidative stress, derailing immune regulation, and distorting thyroid hormone metabolism. When selenium is in short supply, antioxidant enzymes falter, leaving the thyroid gland vulnerable to damage. Low vitamin D blunts immune self-control and fuels pro-inflammatory cells. Iron deficiency - evident as low ferritin - amplifies symptoms because an overactive thyroid cranks up the body’s iron demand. Replenish vitamin D with fatty fish like salmon or tuna, fish-liver oil, egg yolks and beef liver; fortify selenium stores with Brazil nuts, seafood and eggs; and raise ferritin by adding red meat, poultry, fish, legumes, dark leafy greens, nuts, seeds, iron-fortified cereals, dried fruit, whole grains and eggs.
- Stress Management: Chronic stress can adversely affect thyroid function. Incorporating stress-reducing practices such as yoga, meditation, and deep breathing exercises can be beneficial. Regular, moderate exercise, such as walking or swimming, also supports overall wellbeing.
- Lifestyle Modifications: Mindfulness-based stress reduction improves cortisol curves and overall quality of life.
How can we help?
As with hypothyroidism, an accurate and functional assessment is essential for effective management of hyperthyroidism. Serum TSH, fT4, fT3, and thyroid-receptor antibodies (TRAb) determine baseline severity and guide the appropriateness of herbal medicine. We check selenium, vitamin D and ferritin levels, as deficits worsen symptom load and autoimmunity. Blood tests and imaging - ultrasound and radioactive iodine uptake (RAIU) scans - are crucial diagnostics in differentiating the cause.
Managing hyperthyroidism through naturopathic medicine involves a comprehensive approach that includes a moderate iodine and antioxidant diet, evidence-based herbal medicine, and management of lifestyle factors such as stress, sleep hygiene and emotional wellbeing. By focusing on the body’s innate healing capacity, naturopathy aims to restore balance and improve the quality of life for those affected by hyperthyroidism.
If you’re experiencing symptoms of hyperthyroidism, speak to All Naturopath today.
Call us today at 0402 926 675 for an appointment!
